Article prepared by Leighton Bradgate
What is OA?
Sometimes called degenerative joint disease or degenerative arthritis osteoarthritis (OA) is the most common chronic condition of the joints, causing large amounts of disability and pain in the Australian community. OA can affect any joint, but it occurs most often in the knees, hips and the small joints of the hands and the base of the big toe. ,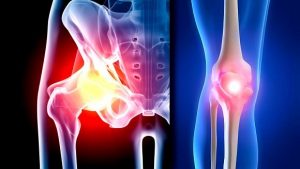 In normal joints, a firm, rubbery material called cartilage covers the end of each bone. Cartilage provides a smooth, gliding surface for joint motion and acts as a cushion between the bones. In OA, the cartilage gradually breaks down, causing pain, swelling and problems moving the joint. In the final stages of OA, the cartilage wears away and bone rubs against bone leading to joint damage and more pain.
In normal joints, a firm, rubbery material called cartilage covers the end of each bone. Cartilage provides a smooth, gliding surface for joint motion and acts as a cushion between the bones. In OA, the cartilage gradually breaks down, causing pain, swelling and problems moving the joint. In the final stages of OA, the cartilage wears away and bone rubs against bone leading to joint damage and more pain.
Who is affected?
Although OA occurs in people of all ages, it is most common in people older than 65. Currently one in two adults will develop symptoms of knee OA during their lives. One in four adults will develop symptoms of hip OA by age 85. The incidence of this pathology is expected to dramatically increase over the next 2 decades. There is a strong correlation between obesity and OA. The mechanism(s) by which obesity contributes to the onset and progression of OA are not fully understood. The strong association between body mass index, altered limb alignment, and OA of the hip and knee support the hypothesis that the effects of obesity on the joint are due to increased biomechanical loading and associated alterations in gait. However recent studies suggest that metabolic factors associated with obesity alter systemic levels of pro-inflammatory cytokines that are also associated with OA. Previous joint injury including ligament sprains, joint dislocations, fractures and cartilage tears associated with the hip and/or knee as well as overuse of these joints can also predispose one to OA. Research has indicated that up to 1.6 times your body weight travels through your joints during slow walking whilst 3 times to 5 times your body weight travel through your joints whilst running. Finally genetic factors have been found to be strong determinants of the disease. Evidence of a genetic influence of OA comes from a number of sources, including epidemiological studies of family history and family clustering, twin studies, and exploration of rare genetic disorders
Signs and Symptoms
- Joint pain and swelling.
- Pain increases when you are active (especially walking, up/down stairs, in/out cars, in/out chairs), but gets a little better with rest.
- Feeling of warmth in the joint.
- Stiffness, especially in the morning or when you have been sitting for a while
- Crepitus when the joint moves
Management
There is currently no cure for OA. Treatment is aimed primarily at symptom relief, improving joint mobility, function and optimising quality of life. According to extensive clinical research exercise therapy is very effective in reducing OA pain. Specifically, exercises that address the weakness and wasting of the knee and hip muscles play a key role in the physiotherapy management of patients with OA hip and/or knee. Pilates is one form of exercise therapy that can help address both the postural variants and muscle weakness patterns commonly seen in patients with OA hip and/or knee. Other techniques such as manual therapy, acupuncture, taping/bracing, walking appliances and activity modification may also be useful adjuncts in managing a patient with OA of the hip and/or knee.
Suitable Analgesia and non-steroidal anti-inflammatory medications are often required in the management of OA in the hip and knee. In more severe cases intra-articular corticosteroid injections are prescribed. These options should be discussed with your GP.
In more severe cases, where conservative management has failed, joint replacement surgery often needs to be considered and is generally able to provide significant relief of symptoms.
If you are suffering OA hip and/or knee, contact your physiotherapist for advice on management of your symptoms.
