 An Australian study found that over a three-month period, 50% of women aged 45-59 years of age experienced some degree of mild, moderate or severe urinary incontinence. It is reported that 65% of women and 30% of men sitting in a GP waiting room report some type of urinary incontinence, yet only 31% of these people report having sought help from a health professional.
An Australian study found that over a three-month period, 50% of women aged 45-59 years of age experienced some degree of mild, moderate or severe urinary incontinence. It is reported that 65% of women and 30% of men sitting in a GP waiting room report some type of urinary incontinence, yet only 31% of these people report having sought help from a health professional.
Urinary incontinence is a term that describes any accidental or involuntary loss of urine from the bladder. Although we can joke by calling it a “wee” problem, urinary incontinence is not a small issue. Stress urinary incontinence (SUI), the most common type of incontinence, is defined as the involuntary loss of urine on effort or physical exertion. This includes leakage with activities such as lifting or lunging, or can occur with sneezing, coughing, or laughing.
Leakage has been thought of as an acceptable side-effect of becoming a mother, or part of the normal aging process. Leakage may be common, however, it is never normal. And, more importantly, up to 90% of urinary incontinence can be cured by following a simple appropriate exercise program. The best time to regain control over your bladder is when leakage first starts.
Anatomy & Physiology
Stopping the flow of urine is the job of your pelvic floor muscles and your urethral sphincter, which are both under your voluntary control.
The pelvic floor is like a sling or hammock of muscular and fibrous tissue that goes from your tailbone to your pubic bone and supports the organs above, such as the uterus, bladder, and rectum. The pelvic floor muscles and sphincters work to close your bladder and urethra, vagina and anus. You can draw these muscles up voluntarily to provide support during additional load, such as running, lifting or sneezing and should tighten automatically with your deep ‘core’ muscles are engaged.
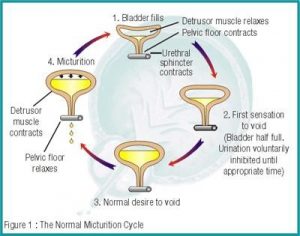 The urethral sphincter mechanism acts like a drawstring which squeezes the urethra shut and stops the urine escaping from the bladder. Your pelvic floor muscle help it to ‘hold on tight’ when you cough, sneeze, laugh or run. Each time it does this, it fires off a reflex which travels from the pelvic floor back to the bladder and tells the muscles of the bladder to stop contracting and trying to push out urine. As the sphincter and pelvic floor muscles relax, another reflex fires, this time telling these muscles to contract.
The urethral sphincter mechanism acts like a drawstring which squeezes the urethra shut and stops the urine escaping from the bladder. Your pelvic floor muscle help it to ‘hold on tight’ when you cough, sneeze, laugh or run. Each time it does this, it fires off a reflex which travels from the pelvic floor back to the bladder and tells the muscles of the bladder to stop contracting and trying to push out urine. As the sphincter and pelvic floor muscles relax, another reflex fires, this time telling these muscles to contract.
As the bladder fills, nerve endings in the wall of the bladder tell you when you are getting close to full. When you are ready the muscles of the pelvic floor and urethral sphincter relax, the bladder muscle contracts until all the urine is passed, then the pelvic floor contracts and the outlet is closed. This can be compared to a river filling a dam. Think of your bladder as a reservoir which is being filled slowly by the river (kidneys above). When the storage in the bladder reaches a certain level, the “hold on” mechanisms let go and urine is pushed out until the bladder is empty. The “hold on” mechanisms take over again and the bladder slowly fills once more.
Maintaining Continence
Maintaining continence requires balance between the pressure within the bladder, and the force on the urethral lumen to keep it closed. In order to maintain urinary continence, the pressure inside the bladder must be less than the force holding the urethra closed. Stress urinary incontinence occurs when the pressure keeping the urethra closed is not enough to counteract the increase in pressure within the bladder. With activities such as coughing, sneezing and lifting, there is an increase in pressure within the abdomen, which inadvertently puts pressure on the bladder. If the pelvic floor muscles are not working well, or are too weak, urine or even faeces may leak out with any increase in pressure.
In addition to weak pelvic floor muscles, SUI can also result from issues within the urethra itself, or may be related to the supportive tissues around the urethra.
Physiotherapy Management of SUI
The primary physiotherapy management of SUI is pelvic floor muscle training, with or without adjunct treatments, such as biofeedback, electrical stimulation, vaginal cones, and support devices.
The aim of physiotherapy is to facilitate and strengthen the pelvic floor muscles. A strong contraction of the pelvic floor muscles will increase the pressure in the urethra as it is pressed against the pubic symphysis. Pelvic floor muscle training should target strength, endurance, co-ordination, or a combination of all three components depending on the condition and presentation. Performing pelvic floor exercises during pregnancy may reduce delivery trauma and accelerate post-partum recovery, and have benefits for long-term pelvic floor function in women. In addition to improving pelvic floor muscle strength and activation, learning the co-ordination of tightening your pelvic floor muscles in preparation for a sudden increase in intra-abdominal pressure has shown to immediately reduce leaking.
There are a variety of biofeedback tools that can be used to assist in training an appropriate pelvic floor contraction. These include pressure biofeedback (Peritron), cones or vaginal weights. Progressing to using weights can improve muscle bulk and strength once you have plateaued with pelvic floor muscle training alone. Cones are a very passive form of treatment that can be done while performing other daily activities, making it easy to integrate into a daily routine.
The pelvic floor needs to be understood and exercised correctly to ensure it will continue to function efficiently throughout your life. Some older women may feel that it is too late to start pelvic floor exercises, yet they are just as likely to benefit and often see great results with pelvic floor retraining.
Mechanical devices, such as a Contiform, can be used to support the urethral position. The Contiform is an intravaginal device made from medical grade elastomer material, which can be worn all day and simply removed for cleaning at night. The Contiform offers an alternative to surgery, particularly in those who not only leak during sport, or those who have not completed their family.
