By Leighton Bradgate October 2014
An anterior cruciate ligament injury (ACL injury) is one of the most common knee injuries in sport. Those who participate in high demand sports involving sudden change of direction like soccer, football, and basketball are more likely to injure their ACL.
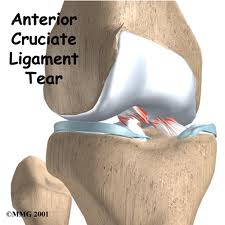
Anatomy of an ACL injury
 Three bones meet to form your knee joint: your thighbone (femur), shinbone (tibia), and kneecap (patella). Your kneecap sits in front of the joint to provide some protection.
Three bones meet to form your knee joint: your thighbone (femur), shinbone (tibia), and kneecap (patella). Your kneecap sits in front of the joint to provide some protection.
Bones are connected to other bones by ligaments. There are four primary ligaments in your knee. They act like strong ropes to hold the bones together and keep your knee stable.
Collateral Ligaments: These are found on the sides of your knee. The medial collateral ligament is on the inside and the lateral collateral ligament is on the outside. They control the sideways motion of your knee and brace it against unusual movement.
Cruciate Ligaments: These are found inside your knee joint. They cross each other to form an “X” with the anterior cruciate ligament in front and the posterior cruciate ligament in back. The cruciate ligaments control the back and forth motion of your knee.
The ACL runs diagonally in the middle of the knee. It prevents the tibia from sliding out in front of the femur, as well as provides rotational stability to the knee.
About half of all ACL injuries are accompanied with damage to other structures in the knee, such as articular cartilage, meniscus, or other ligaments.
Injured ligaments are considered “sprains” and are graded on a severity scale.
Grade 1: The ligament is mildly damaged. It has been slightly stretched, but is still able to help keep the knee joint stable.
Grade 2: The ligament is stretched to the point where it becomes loose. This is often referred to as a partial tear of the ligament.
Grade 3: This type of sprain is most commonly referred to as a complete tear of the ligament. The ligament has been split into two pieces, and the knee joint is unstable.
Partial tears of the ACL are rare; most ACL injuries are complete or near complete tears.
Cause:
- The ACL can be injured in several ways:
- Changing direction rapidly
- Stopping suddenly
- Landing from a jump incorrectly
- Direct contact or collision, such as a football tackle
Several studies have shown that female athletes have a higher incidence (3:1) of ACL injury than male athletes in certain sports. It has been proposed that this is due to differences in physical conditioning, muscular strength, and neuromuscular control. Other suggested causes include differences in pelvis and lower extremity (leg) alignment, increased looseness in ligaments, and the effects of estrogen on ligament properties.
Symptoms:
- Audible “popping” noise at the time of injury, with knee giving way from underneath you.
- Pain and swelling (usually quite significant swelling).
- Loss of full range of motion.
- A feeling of instability or giving way of the knee.
- Discomfort while walking.
If you suffer any of the above symptoms or suspect a serious knee injury you should attend your physiotherapist for assessment. Most ligament injuries can be diagnosed with a thorough examination of the knee. Your physiotherapist may request imaging such as MRI scans to confirm the diagnosis.
Management:
Management for an ACL injury will vary depending upon the patient’s individual needs. For example, the young athlete involved in agility sports will most likely require surgery to safely return to sports. The less active, usually older, individual may be able to return to a quieter lifestyle without surgery.
Nonsurgical Treatment
A torn ACL will not heal without surgery. But nonsurgical treatment may be effective for patients who are elderly or have a very low activity level.
If the overall stability of the knee is intact, your orthopedic surgeon may recommend simple, nonsurgical options including bracing, use of crutches and physiotherapy for a careful rehabilitation and strengthening program.
Surgical Treatment – Rebuilding the ligament
Most ACL tears cannot be sutured (stitched) back together. To surgically repair the ACL and restore knee stability, the ligament must be reconstructed. This procedure is done via an arthroscopy using small incisions.
Your surgeon will replace your torn ligament with a tissue graft. This graft acts as scaffolding for a new ligament to grow on. Grafts can be obtained from several sources. Often they are taken from the patellar tendon or hamstring tendon. Cadaver graft (allograft) can also be used.
Whether or not you undergo surgery, rehabilitation plays a vital role in getting you back to your daily activities. Because the regrowth of the graft takes time, it is recommended that patients undergo at least six months of rehabilitation with a return to sport time frame between nine to twelve months post-surgery.
If you have surgery, physiotherapy first focuses on returning motion to the joint and surrounding muscles. This is followed by a strengthening program designed to protect the new ligament. This strengthening gradually increases the stress across the ligament. The final phase of rehabilitation is aimed at a functional return tailored for the athlete’s sport.